
Video otoscopy (VO) continues to gain acceptance as an integral component of hearing health care practice today. The technologically advanced video-optical technique has applications in the examination, display and documentation of the external ear canal and tympanic membrane. VO is a simple, compact unit incorporating a rod otoscope with a removable otic speculum, fiber-optic illumination, and a high-resolution color video camera capable of recording a patient's ear canal and tympanic membrane.
The technology was introduced to the marketplace nearly five years ago. Roy F. Sullivan, PhD, CCC-A, co-owner of Sullivan and Sullivan, Inc., in Garden City, NY, was among the first audiologists to incorporate VO in an audiology practice. To help audiologists around the world understand the benefits of VO in hearing health care, Dr. Sullivan maintains a website on the World Wide Web to disseminate the most current information on the practical benefits of VO technology.
By projecting an image onto a video monitor, the video otoscope allows the audiologist to compare the status of the ear canal and tympanic membrane before and after treatment, Dr. Sullivan explained. VO also allows patients to - the pinna, concha, ear canal and tympanic membrane during the examination. Audiologists, can use the video otoscope to produce a permanent Polaroid-type photoprint or printout from a computer ink-jet printer that can be transmitted by modem. Images also can be stored on computer disk or videotape. Most VO systems allow the user to freeze, split and strobe frames.
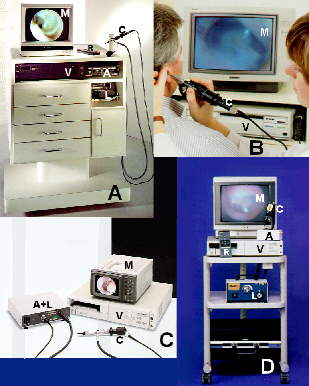
According to Dr. Sullivan, VO instrumentation is available in both clinical and portable models from a number of manufacturers, including Grason-Stadler (Welch Allyn), of Milford, NH; Siemens Hearing Instruments, Inc., of Piscataway, NJ; MedRx, Inc., of Seminole, FL; Rexton Inc., of Plymouth, MN; Starkey Laboratories, Inc., of Eden Prairie, MN; and Interpersonal Communications, of Santa Barbara, CA.
"VO is still not fully reimbursable for audiologists because it is considered an adjunctive tool," he said, "but it goes far beyond what traditional otoscopy offered. The number of things you can do using VO in an audiology practice more than makes up for the cost of the device. VO is the direction our field is heading toward."
While approximately 4,000 video otoscopes have been sold in this country alone, Dr. Sullivan told ADVANCE, many audiologists remain unclear on how to optimize the benefits of the technology. "There still is no graduate or continuing education course which fully prepares a professional for understanding how to use this technology to its fullest potential," he stated. "Audiologists need that extra instruction in ear anatomy and basic medical terminology." Audiologists who understand those anatomical and medical concepts and can communicate that knowledge to physicians by using the video images or printouts provided by VO can gain tremendous respect from referring physicians, Dr. Sullivan said. "You can go to a physician and say, 'This is what I found in my observation,' and show him or her the photos that prove it.
But if audiologists don't have a thorough understanding of the anatomy of the ear and don't possess the medical vocabulary to describe what they find, physicians won't understand what they're talking about and will lose confidence in them. "Someone who only uses Vo to point out the amount of cerumen is spending a lot of money on a tool he or she really isn't benefiting from," he said. Audiologists can use VO in numerous key applications of their practice, including the following:
During the examination process, clinicians can use VO to confirm acoustical and physical access to the external auditory canal (EAC) and the tympanic membrane. "We use VO to identify conditions of the pinna, concha, EAC and tympanic membrane which can hinder acoustic and physical access for audiological diagnostic and hearing aid related procedures," Dr. Sullivan explained. These conditions can include anomalies of the pinna or concha, canal anomalies, tympanic membrane perforations, exogenous factors and endogenous residue.
VO instrumentation also enables audiologists to correlate otoscopic and audiometric findings. "By being able to see what is happening in the ear and making a video or photoprint of the ear canal, we have visual verification of what our pure tone audiometry and tympanometric findings reveal to us," he said. Identifying and monitoring pathology for physician referral are other key functions of VO. "The audiologist is increasingly becoming the professional who serves as the point of entry for patients into the hearing health care system," Dr. Sullivan observed. "As a result, we need to have the tools and basic anatomical and medical knowledge in order to refer a patient on to a physician when warranted. VO helps provide us with that."
As an example, he cited the recent case of a hearing aid user who presented with a suspicious lesion just above the earlobe on the side with the hearing aid. With VO, Dr. Sullivan was able to identify and document the lesion as suspicious and make an appropriate referral to a dermatologist. The subsequent medical diagnosis was squamous cell carcinoma requiring surgical removal and medical treatment. VO is extremely beneficial for identifying conditions that require medical attention such as dermatitis, infections and suspicious growths or neoplasms, he said. It plays an essential role in helping audiologists establish dialogues with physicians on VO observations, especially when related to audiological findings.
VO also can be used to document the efficacy of medical treatment and track treatment outcomes. "I often use VO with patients during their follow-up visits after seeing a physician to see how well an intervention worked,' he said. "We can identify and record on videotape or through Polaroid images the resolution of acute conditions such as otitis extema or otitis media."
Despite the overwhelming amount of video documentation and photographs that can be produced during these exams, audiologists must use the information prudently to encourage more detailed discussions with physicians and otolaryngologists, Dr. Sullivan cautioned. "We must learn to identify and use the proper medical terminology to describe, but not diagnose, the condition(s) we observe in patients using VO," he stated. 'We are not in a position to diagnose medical conditions.' In addition, "we shouldn't just bombard physicians with photographs of various ear structures without documenting what we see and using these images as part of an overall recommendation scheme," he said.
Another benefit of VO is its application in guiding patients through the hearing aid selection process. 'VO is very helpful, in verifying various conditions in the external and middle ear which may influence ear selection of monaural hearing aid fittings," Dr. Sullivan stated. "We use the information we gather of the patient's ear using VO and make hearing aid selection recommendations based on whether the patient has a condition which can prevent him or her from getting an optimal fit."
To ensure the patient will obtain the best results from a hearing aid, it must feel comfortable in the ear and be fitted correctly, Otherwise the aid may cause pain or discomfort, feel unsecured, or cause feedback resulting from an imperfect seal. "You can fit a person with the best hearing aid available, and that person may not benefit from it or even use it regularly if it doesn't feel comfortable to wear," he commented. "By using VO, we can see up close conditions such as the presence of cerumen, desquamation or debris that may cause problems in the impression-taking process. From these observations, he said, audiologists can make recommendations regarding the appropriateness or inappropriateness of a specific hearing aid morphology.
As part of the fitting process, the audiologist can pre-select and verify an oto-block placement site using VO. Having patients open and close their jaw and smile or grimace broadly while the otoscope is placed in the ear canal can provide the practitioner with information on temporomandibular joint (TMJ) and facial muscle movement effects on hearing aid stability, slit leak and feedback presence.
"I also use VO to demonstrate problems that patients may be experiencing with cerumen accumulation," Dr. Sullivan said. "For example, a patient with a new completely-in-the-canal (CIC) hearing aid may come to me complaining that the aid is faulty, when in fact it is buried in cerumen." Using VO, he can show the patient that it isn't the aid that is causing the problem but the cerumen. "From there, I can guide the patient on ways io better manage their cerumen," he said. VO images also provide effective visuals to show patients how the hearing aid is fitted in the ear and how it can be manipulated and operated.
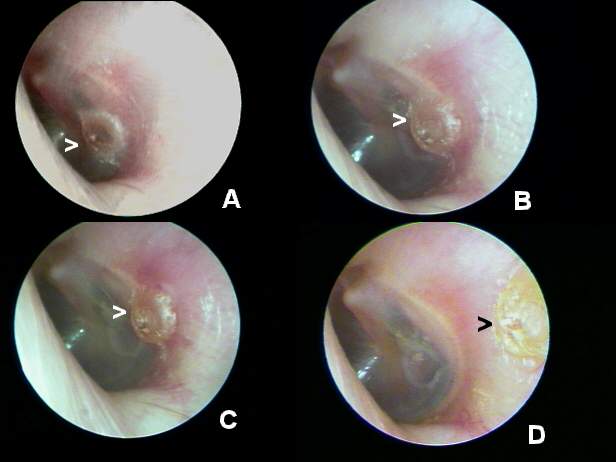
One of the most important benefits of the technology in audiology involves the identification of epidermal irritation loci. While audiologists can use a rod otoscope with a concentric fiber-optical light source to make video oto-endoscopic (VOE) observations of the EAC and tympanic membrane, clinicians can use an enlarged lens to make video oto-macroscopic (VOM) observations of the concha, pinna and peri-auricular areas. VOM observations enable audiologists to see problems such as acute otitis external suspicious growths or neoplasms, nodules and dermatitis. The patient can then be referred to a physician, dermatologist or other specialist for medical diagnosis and treatment.
Utilizing VO to observe and probe, audiologists can identify cerumen accumulation and determine the most appropriate mode of cerumen extraction. Various methods include lavage, suction, curettage, VO-curettage, presoftening with a wetting agent, or a combination of these approaches. VO can be an integral part of a direct or referred CM program. In a referred program, audiologists should use the technique to observe the cerumen impaction and illustrate to the patient why further action is warranted. The nature of the cerumen obstruction can then be documented with a Polaroid or computer VO image printout.
"Far too often we referred a patient to a physician for cerumen removal who afterward told the patient that there really wasn't much build-up," Dr. Sullivan said. "By giving the patient a printout, he or she can see the cerumen obstruction and provide proof to the physician that something needs to be done." During the follow-up visit, the audiologist can verify the post-cerumen remon al status with VO and, if necessary, counsel the patient on proper cerumen self-management techniques. In a direct CM approach, audiologists can use VO to determine the most appropriate mode of extraction depending on the amount of cerumen and its location.
In cases requiring mechanical means to remove cerumen, wax loop accessories can be attached directly to the otoscope head, Dr. Sullivan said. However, video otoscopic monitoring of cerumen removal during irrigation is neither safe nor practical. Afterward VO should Ibe used to verify and document the effectiveness of extraction. Audiologists can routinely monitor cerumen build-up during routine office visits or on a specific follow-up schedule.
"VO ultimately provides the patient with a greater understanding of what is happening in the ear canal and tympanic membrane," he said. "The printouts also let the patient see up close the need for certain actions." For example, a video otoscopic image of a foreign body, such as grains of beach sand lodged in the EAC, ilr lustrate the cause of auditory pain or discomfort, while providing important site-of-acquisition information for the audiologist. "Parents appreciate viewing their child's tubes in situ to see if his or her otitis media, often viewed in the acute stage, has been resolved with medical t treatment," he noted.
Audiologists can use the information they receive using VO to establish greater credibility with patients. "Patients are very impressed when the audiologist hooks up a video otoscope, because they know their physician doesn't have one," Dr. Sullivan said. "Patients consistently comment favorably on the highly apparent technological level of hearing health care practices where video otoscopy is used." The direct visual evidence provided with VO tends to motivate physicians and patients to take action, he said.
In addition, regular use of VO augments the audiologist's knowledge of the variations of normal and pathological anatomy in the external ear and at the tympanic membrane. "The more we have an opportunity to see these structures on video, the greater understanding we will develop over time," Dr. Sullivan stated. "Likewise we improve our CM techniques through constant video self-reinforcement," especially when the cerumen loop is mounted directly on the video otoscope or speculum.
Dr, Sullivan's website is titled "Audiology Forum: Video Otoscopy".
He updates homepage information almost daily to keep up with the demand for new information on VO from audiologists around the world. "The response we have seen to this website has been astronomical," he said. "We have had about 9,000 visits to the website since last September." Approximately 5,000 people have logged on to the site just within the last three months. Hearing health care professionals from more than 50 countries, including Third World nations, have linked to the site. "Just the other day I received a response from a professional in Zaire who thanked me for explaining the VO process and for the opportunity the website offers to professionals around the world to discuss issues surrounding video otoscopy," Dr. Sullivan said.
He plans for the Audiology Forum website to be sponsored as a continuing education and medical information site that professionals and graduate students can take for credit. "It's been a laborious and costly process, but using the Internet has been an extremely successful way to get important information out to other professionals about video otoscopy," Dr. Sullivan said. "The feedback I have received from professionals around the world has been extremely gratifying."